Research Outcomes
ROI researchers are generating results that are advancing practice and improving outcomes for patients. Innovative clinicians developed the resources listed below with grants supported by ROI donors, and thousands of providers are using them to enhance patient care.
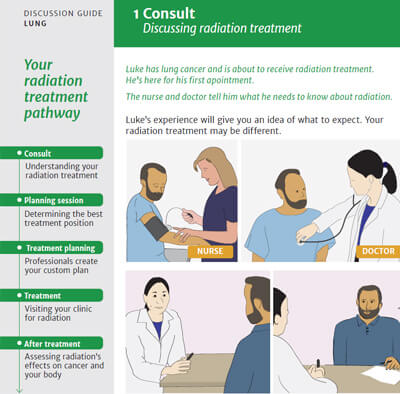
CEBRE Discussion Guides
Daniel Golden, MD, MHPE, created the “Communicating the External Beam Radiotherapy Experience” (CEBRE) series of discussion guides to facilitate conversations between patients and providers. With support from ROI, Dr. Golden’s team developed CEBRE guides about radiotherapy for breast, central nervous system, digestive system, head and neck, lung, and prostate cancers. Visit the CEBRE website for more information about the entire series, and download the discussion guides that were developed with support from ROI below.
- CEBRE Breast Cancer Discussion Guide
- CEBRE Central Nervous System Discussion Guide
- CEBRE Digestive System Discussion Guide
- CEBRE Head and Neck Discussion Guide
- CEBRE Lung Cancer Discussion Guide
- CEBRE Prostate Cancer Discussion Guide
Dr. Golden's team also translated the CEBRE discussion guides into Spanish. Download these guides below, and learn more about the initiative on the CEBRE en Español website.
- CEBRE en Español Breast Cancer Discussion Guide
- CEBRE en Español Central Nervous System Discussion Guide
- CEBRE en Español Digestive System Discussion Guide
- CEBRE en Español Head and Neck Discussion Guide
- CEBRE en Español Lung Cancer Discussion Guide
- CEBRE en Español Prostate Cancer Discussion Guide
RadOnc Toolbox
A free resource for health care professionals provided by ROI, the RadOnc Toolbox puts point-of-care tools at users' fingertips. The app offers easy access to staging, contouring, dose constraints, calculators, toxicity scales, clinical practice guidelines and more to support evidence-based practice. The RadOnc Toolbox was originally developed by Malolan Rajagopalan, MD, MBA, with a grant from ROI in 2014. ROI overhauled the RadOnc Toolbox in 2023 in partnership with Matthew Culbert, MD, and Colton Ladbury, MD, to upgrade the resources and enhance the user experience. Discover the power of the RadOnc Toolbox:
Publications
ROI researchers have published the results of their ROI-supported projects in a wide variety of peer-reviewed journals. Examples of recent manuscripts are included below.
Chao M, Tomalin L, Wei J, et al. Exploring Spatial Dose Information in the Parotid Gland for Xerostomia Prediction and Local Dose Patterns in Head and Neck Cancer Radiotherapy. Biomed Phys Eng Express. 2025 Feb 11;11(2). doi: 10.1088/2057-1976/adb15e.
Lichter KE, Larson B, Pagdala M, et al. Impact of declared wildfire disasters on survival of lung cancer patients undergoing radiation. Cancer Causes Control. 2025 Jan 9. doi: 10.1007/s10552-024-01949-2.
Hughes RT, Prasad JJ, Razavian NB, et al. “If You’re Talking, I Think You’re Muted”: Follow-up Analysis of Weekly Peer Review Discussion and Plan Changes After Transitioning From Virtual to In-Person Format. Clin Oncol (R Coll Radiol). 2024 Dec;36(12):809-816. doi: 10.1016/j.clon.2024.09.006.
Clark M, Harms J, Vasyltsiv R, et al. Quantitative, Real-time Scintillation Imaging for Experimental Comparison of Different Dose and Dose Rate Estimations in UHDR Proton Pencil Beams. Med Phys. 2024 Sep; 51(9):6402-6411. doi: 10.1002/mp.17247.
Chaunzwa TL, Qian JM, Li Q, et al. Body Composition in Advanced Non-Small Cell Lung Cancer Treated With Immunotherapy. JAMA Oncol. 2024 Jun 1;10(6):773-783. doi:10.1001/jamaoncol.2024.1120.
Friesner ID, Feng J, Kalnicki, S, et al. Machine Learning–Based Prediction of Hospitalization During Chemoradiotherapy With Daily Step Counts. JAMA Oncol. 2024 May 1;10(5):642-647. doi:10.1001/jamaoncol.2024.0014.
Wang Y, Deng W, Lee D, et al. Age Associated Disparity in Phagocytic Clearance Affects the Efficacy of Cancer Nanotherapeutics. Nat. Nanotechnol. 2024 Feb;19(2):255-263. doi: 10.1038/s41565-023-01502-3.
Chen X, Mumme RP, Corrigan KL, et al. Deep Learning–based Automatic Segmentation of Cardiac Substructures for Lung Cancers. Radiother Oncol. 2024 Feb:191:110061. doi: 10.1016/j.radonc.2023.110061.
Kamran SC, Zhou Y, Otani K, et al. Genomic Tumor Correlates of Clinical Outcomes Following Organ-Sparing Chemoradiation Therapy for Bladder Cancer. Clin Cancer Res. 2023 Dec 15;29(24):5116-5127. doi: 10.1158/1078-0432.CCR-23-0792.
Lichter KE, Baniel CC, Do I, et al. Impacts of Wildfire Events on California Radiation Oncology Clinics and Patients. Adv Radiat Oncol. 2023 Oct 22;9(3):101395. doi: 10.1016/j.adro.2023.101395.
Lamba N, Cagney DN, Catalano PJ, et al. A Genomic Score to Predict Local Control Among Patients with Brain Metastases Managed with Radiation. Neuro Oncol. 2023 Oct 3;25(10):1815-1827. doi: 10.1093/neuonc/noad098.
Mattes MD, Munoz SM, Thomas CR, and Deville C. Pilot Study Exploring the Feasibility of Incorporating Radiation Oncology into Preexisting Early Pathway Programs for Diverse Premedical Students. Int J Radiat Oncol Biol Phys. 2023 Aug 1;116(5):992-998. doi: 10.1016/j.ijrobp.2023.01.023.
Paradis KC, Franco I, Ponce SB, et al. The Current State of Departmental Diversity, Equity, and Inclusion Efforts Within US Academic Radiation Oncology Departments. Int J Radiat Oncol Biol Phys. 2023 Jun 1;116(2):219-228. doi: 10.1016/j.ijrobp.2022.06.071.
Avila S, Franco I, Bregio C, et al. Spanish Adaptation and Evaluation of Clinical Discussion Guides: Communicating the External Beam Radiotherapy Experience (CEBRE) en Español. Int J Radiat Oncol Biol Phys. 2023 May 1;116(1):166-175. doi: 10.1016/j.ijrobp.2023.01.031.
Madueke I, Lee RJ, and Miyamoto DT. Circulating Tumor Cells and Circulating Tumor DNA in Urologic Cancers. Urol Clin North Am. 2023 Feb;50(1):109-114. doi: 10.1016/j.ucl.2022.09.010.
Mattes MD, Gayed G, Thomas CR, and Deville C. Impact of a Virtual Introduction to Radiation Oncology Presentation on Stimulating Interest in the Specialty Among Diverse Medical Students at Multiple Institutions. J Am Coll Radiol. 2023 Feb;20(2):243-250. doi: 10.1016/j.jacr.2022.10.009.
Kishan AU, Steigler A, Denham JW, et al. Interplay Between Duration of Androgen Deprivation Therapy and External Beam Radiotherapy with or without a Brachytherapy Boost for Optimal Treatment of High-risk Prostate Cancer: A Patient-Level Data Analysis of 3 Cohorts. JAMA Oncol. 2022 Mar 1;8(3):e216871. doi:10.1001/jamaoncol.2021.6871.
Mattes M and Deville C. A survey to assess and delineate approaches to medical student outreach to promote diversity at academic radiation oncology programs. Int J Radiat Oncol Biol Phys. 2022 Apr 1;112(5):1083-1089. doi.org/10.1016/j.ijrobp.2021.12.165.
Ibrahim EH, Frank L, Baruah D, et al. Value CMR: Towards a comprehensive, rapid, cost-effective cardiovascular magnetic resonance imaging. Int J Biomed Imaging. 2021 May 15:2021:8851958. doi: 10.1155/2021/8851958.
Qu XM, Chen Y, Zaric GS, et al. Is SABR cost-effective in oligometastatic cancer? An economic analysis of the SABR-COMET randomized trial. Int J Radiat Oncol Biol Phys. 2021;109(5): 1176-1184. doi: 10.1016/j.ijrobp.2020.12.001.
Tang C, Lei X, Smith GL, et al. Influence of geography on prostate cancer treatment. Int J Radiat Oncol Biol Phys. 2021 Apr 1;109(5):1286-1295. doi: 10.1016/j.ijrobp.2020.11.055.
Paul S, Bodner WR, Garg M, Tang J, Ohri N. Cardiac irradiation predicts activity decline in patients receiving concurrent chemoradiation for locally advanced lung cancer. Int J Radiat Oncol Biol Phys. 2020 Nov 1;108(3):597-601. doi: 10.1016/j.ijrobp.2020.05.042.
Han P, Hales R, Lakshminarayanan P, et al. Exploring the Relationship of Radiation Dose Exposed to the Length of Esophagus and Weight Loss in Patients with Lung Cancer. Pract Radiat Oncol. 2020 Jul-Aug;10(4):255-264. doi: 10.1016/j.prro.2020.03.002.
Tang C, Lei X, Smith GL, et al. Costs and complications after a diagnosis of prostate cancer treated with time-efficient modalities: An analysis of national Medicare data. Pract Radiat Oncol. 2020 Jul-Aug;10(4):282-292. doi: 10.1016/j.prro.2020.02.014.
Nugent SM, Golden SE, Hooker ER, et al. Longitudinal health-related quality of life among individuals considering treatment for stage I non-small-cell lung cancer. Ann Am Thorac Soc. 2020 Aug;17(8):988-997. doi: 10.1513/AnnalsATS.202001-029OC.
Wolfe AR, Wald P, Webb A, et al. A microRNA-based signature predicts local-regional failure and overall survival after pancreatic cancer resection. Oncotarget. 2020 Mar 10;11(10):913-923. doi: 10.18632/oncotarget.27496.